Today we’re talking about Shin splints. So what is to follow is a custom made Rehab program that I created for one of our practice members that let me know that he was having some shin splints.
That’s going to have everything you need for the do it yourself approach at home. But first, let’s talk a little bit about Shin splints. What causes them, what they are, because that is what infers how we manage it.
The underlying etiology is what dictates the exercises that we are going to do to try and prevent this and stop this from happening. So let’s get into it.
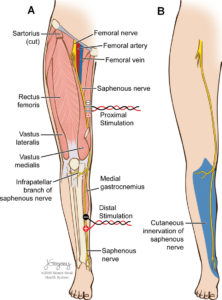
So Shin splints, what are they? It is when you get pain on the lower two thirds or lower half of the inside of the shin. So that’s on the posterior-medial, the back and inside border of the Tibia bone. The Tibia bone is the big shinbone.
If you have ever hit your shin bone then you know it really hurts and shin splints really, really hurt. They’re also tough to manage because it is an injury to the actual bone from muscles like the soleus and the flexor digitorum longus yanking on the layering or the wrapping around the bone called the periosteum.
And we know from studies that it actually involves the bone itself, the cortical bone. So that’s why it really hurts. That’s why it’s tough to manage. And so there are a few factors that we know that lead to shin splints.
The best predictive factor is if you run really fast and you run a lot. If you are a high volume, a high quality or good runner, you’re more likely to get this. But that doesn’t mean that you can’t get it if you’re just an everyday Joe like me who likes to run.
And so there are a few factors that we know can lead to this.
So number one is poor running mechanics.
Number two is a smaller tibia bone, which means more force is absorbed by less bone weakness or stiffness in the calf.
Thirdly, too much movement and weakness in the hip muscles.
Fourthly, poor proprioception, which is the brain-body connection. Your body’s awareness of how the leg, the ankle, and the hip are moving plays an important role in your gait, how you run, your susceptibility to injury and shin splints.
These factors really dictate all the things that we need do need to do to manage it.
Number one, because of that high volume or high speed, we’re going to need to rest. If you have this issue, you’re going to have to rest until it’s no longer painful or you’re able to run in a pain-free manner.
Number two, what we need to do is we need to change the way that you run. You’re going to have to get some coaching or learn to run a bit differently, likely absorbing more force by landing on the midfoot instead of the heel. Also, we know that orthotics work really, really well for this condition.
Why? Because you slip an orthotic in, it’s going to increase your PROPRIOCEPTION and automatically change the way the foot moves and change the way that you run.
The next thing that we need to do is we need to have more force absorption and better force absorption of the impact that is going up into the body so that it doesn’t go into the Tibia bone. We want it to go into the muscles, so that’s where we’re going to spend some time stretching and strengthening the calf, which you will see in the Rehab Protocol (below) in order to also improve our gait mechanics or our running.
We also want to improve our hip strength and flexibility and so that’s where you’ll see some work on the internal and external rotators of the hip. That’s going to improve our body’s ability to again absorb force so it doesn’t go into that Tibia bone.
We also know with this condition that it is associated with lower bone density and so that’s where if you are somebody who has a lower bone density, you might want to try some supplementation that’s going to increase that bone density (vitamin D & calcium) and add more weight-bearing and strengthening exercises to strengthen the bones and the calf muscles and the hips for that matter. This will allow for better force absorption.
And then last but not least, we talked about proprioception and that’s what we do in our office, the brain-body connection.
1)We do that in three ways, making sure the spine is healthy.
2) We do neuro or electroacupuncture to the nerves around the leg, calf, and hip to make sure that the signal is going to and from the leg are healthy.
And then number three, which can also work well for the do it yourself approach. We get people to tape the inside of their leg so that the proprioception is improved there.
So that’s how we manage this condition in our office. Guys, I hope that’s helpful. I hope gives you a little bit more information that you’re going to need to help manage this. If you have any follow up questions, be sure to let me know. If you want us to review your case to help you with this particular issue or maybe some other source of collateral damage from the spine and the nervous system, let us know. We’d be happy to do that. Check out the videos that are to come for the Rehab Protocol, and as always, I hope this helps you get a little bit healthier and this case a little bit faster.